As we venture into the complex terrain of Laser Spine Surgery, understanding its safety measures and potential risks becomes vital. With the advent of advanced laser technology, spinal surgeries have seen radical improvements in precision and recovery times. However, it is equally essential to shed light on potential setbacks such as surgical complications, infection risks, and accidental tissue damage. This discussion aims to offer a thorough perspective on such issues, encouraging an informed dialogue between patients and healthcare providers and facilitating decisions that prioritize safety and effectiveness.
Understanding Laser Spine Surgery
The patient’s comprehension of laser spine surgery—a minimally invasive procedure that utilizes laser technology to treat various spinal conditions—is crucial to making an informed decision about this advanced surgical option. This comprehension is intricately linked to the understanding of spinal anatomy and the different types of lasers used in the procedure.
The spinal anatomy comprises a complex system of bones, muscles, nerves, and other tissues that contribute to our body’s ability to function. Conditions such as herniated discs, spinal stenosis, and spondylolisthesis can cause debilitating pain and limit mobility, often requiring surgical intervention. Laser spine surgery targets these conditions specifically, offering a less invasive alternative to traditional open spine surgeries.
Laser types used in spine surgery vary. CO2 and YAG lasers have historically been used, though their application has become limited due to the risk of thermal damage. Newer technologies employ the use of diode lasers, which provide the surgeon with greater precision and less risk of collateral damage to surrounding tissues. These lasers work to ablate or remove the problematic tissue, relieving the patient’s symptoms and improving their quality of life. Understanding these aspects is crucial to making an informed decision regarding laser spine surgery.
The Evolution of Spinal Surgeries
Delving into the history of spinal surgeries, it becomes evident that major advancements and refinements have profoundly altered the landscape of these procedures over the years. Initially, spinal surgery history was marked by invasive open surgeries, often leading to significant pain, lengthy recoveries, and considerable risk.
As the medical field advanced, so did the techniques used in spinal surgeries. The implementation of microsurgery in the late 20th century was a significant milestone. This approach, using specialized microscopes and miniature surgical tools, allowed for more precise surgical work, reducing damage to surrounding tissues.
The dawn of the 21st century brought about modern surgical advancements that further revolutionized spinal procedures. Endoscopic spine surgery, for instance, utilizes small incisions and a camera to guide the procedure, thereby reducing operative trauma and enhancing patient recovery.
The latest evolution in this field is laser spine surgery, a minimally invasive technique employing laser technology to treat spinal conditions. This advancement represents the culmination of a long journey, from invasive open surgeries to minimally invasive procedures, embodying the constant pursuit of safer, more effective treatment methods within the domain of spinal surgery history.
Key Benefits of Laser Spine Surgery
Embracing the cutting-edge technology of lasers, spine surgery has witnessed notable improvements regarding patient safety, recovery time, and overall effectiveness. Laser spine surgery provides a minimally invasive solution for patients suffering from spinal conditions. This advanced surgical technique reduces trauma to surrounding tissues, leading to less postoperative pain and a quicker return to daily activities.
One of the key benefits of laser spine surgery is the reduction of surgery costs. Traditional open spine surgery often requires extended hospital stays and lengthy rehabilitation periods, significantly increasing the financial burden on patients. On the other hand, laser spine surgery is often performed on an outpatient basis, substantially lowering the cost associated with hospitalization. For those considering this innovative procedure consulting a specialist for laser spine surgery can provide a clear understanding of potential benefits and personalized care options.
Additionally, the less invasive nature of laser spine surgery can result in fewer complications and less risk of infection, further reducing potential healthcare costs. This aspect is particularly relevant considering the current healthcare environment where insurance coverage can be a significant factor in a patient’s decision to pursue surgical treatment.
While insurance coverage varies, many insurance companies recognize the benefits of laser spine surgery and provide coverage for this procedure, further enhancing its appeal to patients seeking effective and economical treatment for their spinal conditions.
The Science Behind Laser Technology
Having examined the benefits of laser spine surgery, it’s important to understand the scientific principles that underpin this innovative technology. Central to laser spine surgery is laser physics, a field that studies the properties and behavior of light, particularly its interaction with matter.
Lasers, an acronym for Light Amplification by Stimulated Emission of Radiation, produce a concentrated beam of light with specific energy levels and wavelengths. In spine surgery, this laser beam can vaporize or cut tissue, offering precision that traditional surgical tools often lack. The laser’s beam wavelength and power can be adjusted to target specific tissues, minimizing collateral damage to the surrounding area.
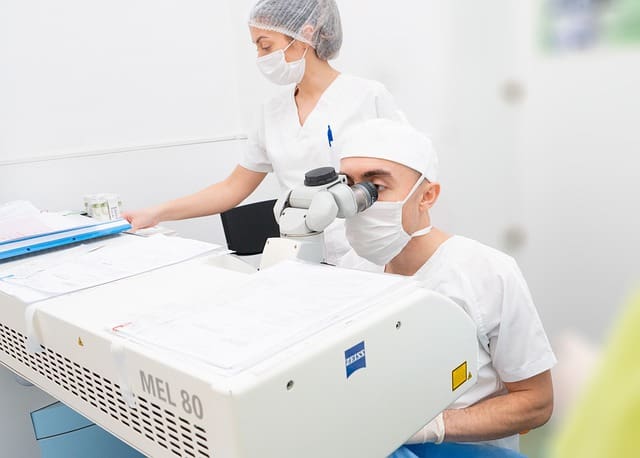
Technology advancements have further refined the use of lasers in spine surgery. Today’s lasers are smaller, more efficient, and offer better control to the surgeon. Innovations in fiber optics have allowed for the integration of lasers with endoscopic technology, enabling surgeons to perform minimally invasive procedures.
Understanding the science behind laser technology helps us appreciate the precision and control it offers. However, as with any surgical intervention, it is critical to weigh these benefits against potential risks to make an informed decision. This balance forms the basis of our next discussion, ‘Potential Risks in Laser Spine Operations.’
Potential Risks in Laser Spine Operations
While laser spine surgery is often heralded for its precision and minimally invasive approach, it is important to fully comprehend the potential risks associated with it. Chief among these are surgical complications, which can arise from the procedure itself, and the risk of postoperative infections, often a concern in any surgical intervention. It is essential to fully understand these risks to make an informed decision about undergoing laser spine surgery.
Understanding Surgical Complications
Despite the precision that laser spine surgery offers, it is imperative to understand that, like any surgical procedure, it carries potential risks and complications. One significant area of concern involves surgical tool sterilization. Even though rigorous sterilization procedures are typically in place, there remains a small chance of contamination, which can lead to serious complications.
Another critical aspect is anesthesia complications, which may occur in a small percentage of patients. These complications can range from minor reactions, such as nausea and dizziness, to significant issues, like allergic reactions or cardiovascular events. An individual’s health history and physical condition can influence their risk.
Moreover, while laser technology allows for minimally invasive procedures, there is still the risk of unintended damage to surrounding tissues. This could potentially lead to complications such as nerve damage or excessive bleeding.
Postoperative Infection Risks
The patient’s journey to recovery following laser spine surgery is not devoid of potential hurdles, with postoperative infections posing a significant risk. Despite stringent sterilization procedures, bacteria can still infiltrate surgical incisions, leading to infection. These microbial invaders may originate from the patient’s skin, contaminated surgical instruments, or airborne pathogens in the operating room.
Infection symptoms such as fever, chills, redness, swelling, increased pain at the surgical site, and pus or foul-smelling drainage are warning signs that should not be ignored. Early detection and treatment of infections can prevent complications and improve the recovery outcome.
Treatment usually involves antibiotics, but the rise of antibiotic resistance is a growing concern. This resistance occurs when bacteria mutate or acquire resistance genes from other bacteria, rendering antibiotics ineffective. The overuse and misuse of antibiotics further exacerbate this problem.
To mitigate this risk, surgeons may use prophylactic antibiotics before and after surgery. However, this should be done judiciously to prevent the development of resistant strains. Additionally, strict adherence to postoperative care instructions, such as wound cleaning and dressing changes, can help minimize the chances of infection. A proactive approach toward infection control is pivotal in ensuring a successful recovery from laser spine surgery.
Preoperative Safety Measures
Before a patient undergoes laser spine surgery, several preoperative safety measures are implemented to mitigate risks and guarantee a successful procedure. This includes meticulously understanding preoperative guidelines, conducting essential medical evaluations, and effectively managing pre-surgery anxiety. Each of these measures plays a significant role in decreasing the likelihood of complications and enhancing the overall safety of the surgery.
Understanding Preoperative Guidelines
Understanding the preoperative guidelines is crucial for maximizing patient safety and surgical outcomes in laser spine surgery. These guidelines include a range of lifestyle adjustments and dietary considerations that contribute towards reducing surgical risk and enhancing postoperative recovery.
Lifestyle adjustments form an integral part of preoperative preparation. Patients may be advised to cease smoking, limit alcohol consumption, and engage in regular physical activity leading up to the surgery. These changes aim to improve overall health, enhance immune response, and promote ideal surgical conditions.
Equally important are dietary considerations. A balanced diet rich in proteins, vitamins, and minerals can aid in wound healing and tissue regeneration after surgery. Certain patients may also be advised to lose weight to reduce stress on the spine and improve surgical outcomes. It’s important to consult with a dietitian to create a personalized preoperative nutrition plan.
Patients should also ensure sufficient hydration while avoiding food and drink close to the surgical procedure, as per anesthesiologist instructions. The goal of these guidelines is to minimize potential complications, such as infection or poor wound healing, and to promote a swift and effective recovery. Adhering to these preoperative guidelines can have a significant impact on the success of laser spine surgery.
Essential Medical Evaluations
An important aspect of preoperative safety for laser spine surgery involves undertaking essential medical evaluations to ascertain the patient’s overall health condition and readiness for the procedure. This rigorous process is vital in ensuring the patient’s body can endure the surgery and recuperate effectively.
Firstly, a thorough medical history is taken, including details of past surgeries, allergies, and chronic conditions. The surgeon also needs to understand the patient’s lifestyle choices, such as smoking and alcohol consumption, as these can have a substantial impact on the surgery’s outcome.
Next, a series of diagnostic tests, including blood tests, imaging studies, and sometimes cardiac evaluations, are performed. These tests provide invaluable information on the patient’s health status and reveal potential risks that might need to be managed proactively.
Patient counseling is another critical component of the preoperative evaluation. During these sessions, the surgeon addresses the patient’s concerns, outlines the procedure in detail, and discusses possible risks and expected outcomes. This helps the patient make an informed decision about the surgery.
Lastly, a review of the patient’s medical insurance is essential. It helps determine what costs are covered, ensuring financial aspects do not become a hurdle in receiving care. Therefore, essential medical evaluations form an integral part of safe and effective preoperative planning.
Managing Pre-surgery Anxiety
Apart from thorough medical evaluations, addressing pre-surgery anxiety is another important aspect of preoperative safety measures that demands attention. Anxiety, if not properly managed, can have a negative impact on a patient’s surgical experience and recovery process. The emotional state of a patient is as crucial to take into account as the physical condition when planning for laser spine surgery.
Several anxiety reduction techniques can be beneficial. These may include mind-body techniques like deep breathing exercises, progressive muscle relaxation, and guided imagery, among others. These are designed to help patients relax and reduce their anxiety levels leading up to the surgery. Additionally, cognitive-behavioral therapy (CBT) can be a useful tool for managing anxiety, as it helps patients understand and change thought patterns that lead to anxiety and fear.
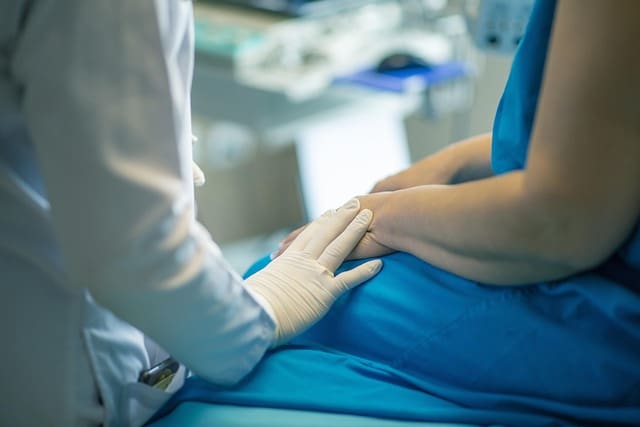
The importance of emotional support cannot be overstated in this situation. A strong support network, including family, friends, and medical professionals, can greatly alleviate pre-surgery anxiety. Emotional support can make a significant difference in a patient’s emotional well-being and overall surgical experience. Hence, it is essential for healthcare providers to recognize and address pre-surgery anxiety as a part of thorough preoperative safety measures.
During the Surgery: What to Expect
Guiding through the complex process of laser spine surgery, patients can expect a range of experiences that typically commence with anesthesia administration to guarantee comfort and painlessness. The effects of anesthesia are manifold, primarily working to numb the area being operated on while also keeping the patient in a state of controlled unconsciousness. Side effects may include temporary confusion or memory loss, but these are usually transitory and not cause for alarm.
The surgery duration is variable, often dependent on the complexity of the patient’s spinal condition and the specific procedure being performed. On average, laser spine surgery may take between one to two hours. Throughout the procedure, a highly trained surgical team monitors the patient’s essential signs to ensure safety and prompt response to any potential complications.
The procedure itself involves creating a small incision in the back, through which a laser is inserted to remove or shrink the offending tissue, causing pain or discomfort. The precision of the laser allows for minimal damage to surrounding tissues, thereby reducing the risk of complications and promoting faster healing. This intricate procedure requires experienced surgeons and state-of-the-art technology, further underscoring the need to choose a reputable healthcare provider.
Postoperative Care and Precautions
Upon completion of laser spine surgery, meticulous postoperative care is crucial to guarantee the best recovery possible. This involves a thorough approach to pain management, with strategies customized to each individual’s needs and responses. Simultaneously, vigilance in preventing postoperative infections is vital, as well as employing strict hygiene protocols and monitoring for early signs of complications.
Pain Management Post-Surgery
Managing pain effectively after laser spine surgery is vital to enhance patient comfort, promote a smooth recovery process, and minimize potential complications. This involves a holistic approach, incorporating various anesthesia options and strategies for chronic pain management.
Anesthesia options for postoperative pain control often include systemic medications, regional techniques, or a combination of both. Systemic medications such as opioids, non-opioid analgesics, and co-analgesics can be administered orally, intravenously, or through patient-controlled analgesia (PCA) pumps. Regional techniques, such as epidural or spinal anesthesia, provide targeted pain relief and may reduce the need for systemic medications, minimizing side effects.
For patients with a history of chronic pain, managing post-surgery discomfort can be more challenging. It is important to devise a personalized pain control strategy that addresses the patient’s unique needs. This might involve a multi-modal approach, combining pharmacological interventions with non-pharmacological methods like physical therapy, cognitive-behavioral therapies, and alternative treatments like acupuncture.
Preventing Infection Risks
Preventing infection postoperatively is a vital aspect of care following laser spine surgery, requiring diligent attention to hygiene, wound care, and the administration of prophylactic antibiotics when necessary. The first step in preventing infection risks is infection source identification. Careful monitoring of the wound and the patient’s overall condition can help in identifying potential sources of infection early.
Antibiotic resistance implications also play a significant role in postoperative infection prevention. The use of antibiotics should be judicious, taking into account the patient’s medical history and the potential risk of developing antibiotic resistance. The presence of antibiotic-resistant bacteria can complicate treatment and prolong recovery.
Additionally, maintaining a sterile environment, both in the operating room and during the recovery period, is essential. Patients should be educated on proper wound care and the importance of regular hand hygiene. Medical staff should adhere to strict infection control protocols, including the use of personal protective equipment.
Long-Term Implications and Recovery
The long-term implications and recovery process associated with laser spine surgery are important considerations that patients must be well-informed about before undergoing the procedure. The rehabilitation processes after surgery typically involve physical therapy, aimed at strengthening the back muscles and promoting spinal flexibility. This process can range from a few weeks to several months depending on the patient’s condition and the complexity of the surgery.
Psychological impacts should not be overlooked. The journey to recovery may be strenuous and can lead to feelings of frustration or depression in some patients. It is, hence, essential for healthcare providers to offer psychological support to help patients cope with this phase.
The success of laser spine surgery in the long-term is generally high, with many patients experiencing significant pain reduction and improved quality of life. However, potential risks such as nerve damage, infection, or recurrence of symptoms may occur. It’s also worth noting that patients with severe degenerative conditions may not experience full relief from symptoms.

Real-Life Stories: Patient Experiences
While understanding the theoretical aspects of recovery is important, examining real-life stories of patients who have undergone laser spine surgery can provide a more thorough picture of what the experience entails. These patient testimonials provide a firsthand account of the procedure, the surgery’s aftermath, and the path to recovery.
One such account comes from a 50-year-old patient who had been suffering from chronic lower back pain for years. Post-surgery, he reported significant relief from his debilitating pain. He was able to return to his job and resume daily activities within a few weeks, reflecting the minimally invasive nature of the procedure.
In another patient testimonial, a 60-year-old woman who underwent surgery for her cervical spine reported improved mobility and reduced discomfort almost immediately. The surgery aftermath, for her, was marked by a rapid recovery and improved quality of life.
However, it’s important to note that experiences can vary. A 35-year-old patient reported mild discomfort in the weeks following the surgery, indicating that recovery times can differ based on individual health conditions and the specific nature of the spinal issue. These narratives underline the necessity of having well-informed, individualized expectations about the surgery and subsequent recovery.
Alternatives to Laser Spine Surgery
Despite the benefits of laser spine surgery, it is not the only option available for patients seeking relief from chronic back or neck pain. Non-surgical treatments often serve as effective alternatives, with the potential to alleviate discomfort and improve functionality.
Physical therapy, for instance, uses targeted exercises and maneuvers to strengthen the body, enhance flexibility, and reduce strain on the spinal structures. Pain management techniques, such as nerve blocks or epidural steroid injections, can also provide temporary relief.
In addition, chiropractic care is another non-surgical approach that focuses on aligning the spine to alleviate pressure on nerves and discs. This treatment modality has shown effectiveness in relieving pain and improving patients’ quality of life.
Holistic approaches, such as acupuncture, yoga, and mindfulness meditation, are increasingly being recognized for their potential in managing chronic pain. These techniques focus on the mind-body connection and can help patients to manage their symptoms better.
Lastly, lifestyle modifications, including a balanced diet, regular exercise, and proper ergonomics, play an essential role in maintaining spine health and preventing further injury. These alternatives, while varied, offer a diverse range of options for patients to explore before resorting to surgery.
Making an Informed Decision
Deciphering through the myriad of treatment options for chronic back or neck pain, patients must make an informed decision, considering both the potential benefits and risks associated with each method. Laser spine surgery, for example, offers a less invasive alternative to traditional open-back surgery, but it’s not without its own set of complications and drawbacks.
A vital component of this decision-making process involves understanding the financial implications. Surgery financing options vary considerably, from self-pay to medical loans to payment plans offered directly by the surgical center. The cost-effectiveness of laser spine surgery should be thoroughly evaluated against its potential health benefits and risks.
Equally important is to verify insurance coverage. Not all insurance companies cover laser spine surgery, as some consider it experimental or not medically necessary. Patients should consult with their insurance provider, ensuring they are well-informed about what is and isn’t covered before moving forward.
Frequently Asked Questions
What Medical Conditions Would Disqualify Me From Undergoing Laser Spine Surgery?
Certain medical conditions such as severe osteoporosis, obesity, or uncontrolled diabetes may disqualify you for laser spine surgery due to potential post-surgery complications and a potentially prolonged recovery timeline. Always consult your doctor for personalized advice.
How Does Laser Spine Surgery Compare in Cost to Traditional Spine Surgery Methods?
Like comparing apples to oranges, laser spine surgery can be more expensive than traditional methods, but this varies depending on insurance coverage. However, its shorter recovery timeline may offset additional costs in the long run.
Are There Any Specific Lifestyle Changes Required Prior to Undergoing Laser Spine Surgery?
Prior to undergoing laser spine surgery, specific lifestyle changes such as dietary modifications for best health and smoking cessation to enhance recovery are typically required. These adjustments aid in successful surgical outcomes and faster recuperation.
What Sort of Training and Qualifications Should a Surgeon Have to Perform Laser Spine Surgery?
A surgeon performing laser spine surgery should have extensive surgical training, board certification, and specific experience in laser procedures. A patient’s evaluation of the surgeon’s experience and credentials is vital for ensuring successful outcomes.
How Does Laser Spine Surgery Affect Mobility and Physical Activity in the Long Term?
Laser spine surgery typically enhances long-term mobility and physical activity due to its precision. However, outcomes can vary based on individual circumstances and the quality of post-surgery rehabilitation.












