Navigating the challenges presented by an infected tooth requires a nuanced understanding of its implications on both oral and overall health. Such infections not only manifest through a spectrum of symptoms ranging from discomfort to acute pain but also pose a risk of escalating into more severe systemic health issues if left untreated.
This guide is meticulously structured to provide a detailed overview of the critical steps involved in identifying, addressing, and preemptively managing tooth infections.
What Is A Tooth Infection?
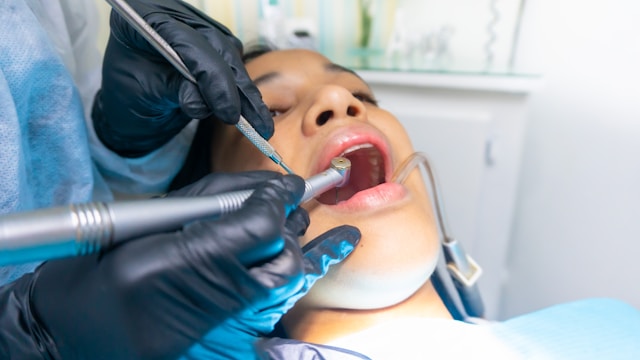
A tooth infection, medically referred to as a dental abscess, occurs when bacteria invade the dental pulp, the innermost part of the tooth containing nerves, blood vessels, and connective tissues. This invasion typically results from untreated dental cavities, injuries, or prior dental work.
The bacteria can cause an infection that may spread to the root of the tooth and beyond, leading to a range of symptoms, including pain, swelling, and the formation of pus. If not treated timely and effectively, such as undergoing a root canal treatment, a tooth infection can lead to more serious health complications.
Types of Tooth Infections
Tooth infections can manifest in several forms, each affecting different parts of the tooth and surrounding tissues. Understanding these types is crucial for identifying the appropriate treatment. Here are the primary types of tooth infections:
1. Dental Caries (Cavities)
Acid produced by bacteria in your mouth damages the hard surface of your teeth, causing dental caries. These bacteria convert sugars in food into acid, which then erodes the tooth enamel, leading to cavities. Without treatment, cavities can progress deeper into the tooth, affecting the dental pulp and causing toothache.
2. Pulpitis
This is an infection of the pulp, the innermost part of the tooth that contains nerves and blood vessels. Pulpitis can be reversible or irreversible. Reversible pulpitis is when the pulp is inflamed but can heal, while irreversible pulpitis means the pulp cannot recover, often leading to a dental abscess if not treated promptly.
3. Periodontal (Gum) Disease
Periodontal disease affects the gums and the bone that supports the teeth. It starts as gingivitis, characterized by red, swollen, and bleeding gums. If not addressed, it can advance to periodontitis, where the inner layer of the gum and bone pull away from the teeth and form pockets. These pockets can become infected, leading to the loss of bone and teeth.
4. Dental Abscesses
A dental abscess is a collection of pus that forms due to a bacterial infection inside the tooth, gums, or bone holding the teeth. There are three main types of dental abscesses:
- Periapical Abscess: Occurs at the tip of the tooth’s root.
- Periodontal Abscess: Found in the gums next to a tooth root.
- Gingival Abscess: Located in the gum tissue and does not affect the tooth or periodontal ligament.
Symptoms of An Infected Tooth

Recognizing these symptoms is crucial for seeking timely dental care, which can prevent the infection from worsening and spreading. Here’s a detailed look at the common symptoms associated with a tooth infection:
1. Pain
Pain from an infected tooth is not just any ordinary toothache. It’s often described as a persistent, throbbing discomfort that can be severe. This pain may radiate to the jaw, neck, or ear on the affected side, highlighting the intensity and potential spread of the infection. Activities such as chewing or applying pressure to the tooth can exacerbate the pain, indicating the tooth’s heightened sensitivity due to the infection.
2. Sensitivity
Sensitivity associated with an infected tooth extends beyond the usual discomfort from cold or hot foods and drinks; it can become a sharp, piercing pain upon exposure to temperature extremes or even sweet, acidic, or spicy foods. This heightened sensitivity signifies that the infection has reached the tooth’s nerve, affecting its response to external stimuli.
3. Swelling
Swelling around an infected tooth often involves the gum tissue but can extend to the face, cheek, or neck, indicating a significant inflammatory response to the infection. This swelling can create a sense of pressure and tenderness in the affected area, making it uncomfortable and sometimes painful to touch or apply pressure.
4. Pus or Discharge
The presence of pus or a discharge is a clear sign of an abscess, a collection of pus due to the infection. This condition may also cause a foul taste in the mouth or persistent bad breath, symptoms that are not alleviated by regular brushing, flossing, or mouthwash, indicating the infection’s severity and the need for professional dental intervention.
5. Fever
Fever, as a symptom of a tooth infection, reflects the body’s systemic response to fight off the infection. A fever might not occur with every tooth infection, but when it does, it indicates that the body is attempting to manage the spread of the infection, signaling the need for immediate dental care.
6. Lymph Node Swelling
Swollen lymph nodes under the jaw or in the neck area occur as the immune system responds to the infection, indicating its attempt to contain and fight off the invading bacteria. Tender and swollen lymph nodes are a sign that the infection may be more serious and widespread than initially thought.
7. Difficulty Opening The Mouth
When an infection leads to significant swelling and pain, it can restrict jaw movement, making it challenging to open the mouth fully or to chew. This limitation not only affects oral function but also signifies the severity of the infection and inflammation, necessitating urgent dental attention.
Treatment And Recovery
Treating an infected tooth and ensuring a smooth recovery involves a multi-faceted approach tailored to the severity of the infection, the affected tooth’s condition, and the patient’s overall health. Here’s a comprehensive overview of the treatment options and recovery processes for tooth infection:
Treatment Options
- Antibiotics
For bacterial infections, antibiotics can be prescribed to reduce and eliminate the bacteria causing the infection. Antibiotics are particularly useful in cases where the infection has spread beyond the tooth, causing swelling and fever. However, antibiotics alone may not address the root cause of the infection inside the tooth.
- Root Canal
A root canal is a common treatment for infected teeth, especially when the infection has reached the pulp (the innermost part of the tooth). In this procedure, the dentist first extracts the infected pulp, then cleans the tooth’s interior, and finally fills and seals it to prevent further infection. This treatment can save the tooth, alleviate pain, and restore its function.
- Tooth Extraction
If the tooth is severely damaged or the infection is extensive and cannot be resolved through other treatments, the dentist may need to extract it. Removing the tooth eliminates the source of infection, and options for replacing the tooth, such as dental implants or bridges, can be discussed after healing.
- Drainage of Abscess
If an abscess forms due to the infection, draining it might be necessary to relieve pain and start the healing process. This is often a preliminary step before further treatment, like root canal treatment or extraction.
Recovery Process
- Post-Treatment Care
After treatment, it’s crucial to follow the dentist’s aftercare instructions closely. This includes taking prescribed medications, such as antibiotics or pain relievers, and avoiding certain foods and drinks that irritate the treated area.
- Oral Hygiene
Maintaining good oral hygiene is essential during recovery. Gentle brushing and flossing, using a soft toothbrush around the treated area, and possibly antiseptic mouthwash can help prevent further infection and promote healing.
- Follow-Up Visits
You may need to visit the dentist for follow-up appointments to monitor the healing process and ensure the infection has been fully resolved. If you underwent a root canal, you might need a final restoration to restore the tooth’s function and appearance fully.
- Pain Management
Some discomfort is normal after treatment for a tooth infection, especially after procedures like tooth extraction or root canal therapy. You can usually manage pain with over-the-counter pain relievers, but following the dentist’s medication recommendations is essential.
- Rest and Nutrition
Resting and avoiding strenuous activities help speed up the recovery process. Eating a healthy, soft food diet can also be beneficial, especially after tooth extraction or when the mouth is sensitive.
Conclusion
The ordeal of a tooth infection, with its potential for significant discomfort and serious health implications, underscores the importance of proactive oral healthcare. By recognizing symptoms early, seeking prompt, professional intervention, and adhering to recommended treatments and preventive practices, individuals can successfully navigate from the pain of infection to the relief of recovery.
Featured Photo by lafayett zapata montero on Unsplash